
Since the start of the COVID-19 pandemic, researchers have been working to better understand and characterize the varied symptoms of the disease. One of the most concerning symptoms is the development of large blood clots that can cause blockages in the arteries that lead to the brain causing stroke.
Researchers at Western University and Lawson Health Research Institute led by Dr. Luciano Sposato have been investigating the relationship between COVID-19 and stroke to better understand the risk in patients and aid in treatment planning. In a new study published in the September 15, 2020 online issue of Neurology, the medical journal of the American Academy of Neurology, the research team reports that approximately two in every 100 patients admitted to hospital with COVID-19 will suffer a stroke, and 35 per cent will die as a result of both conditions.
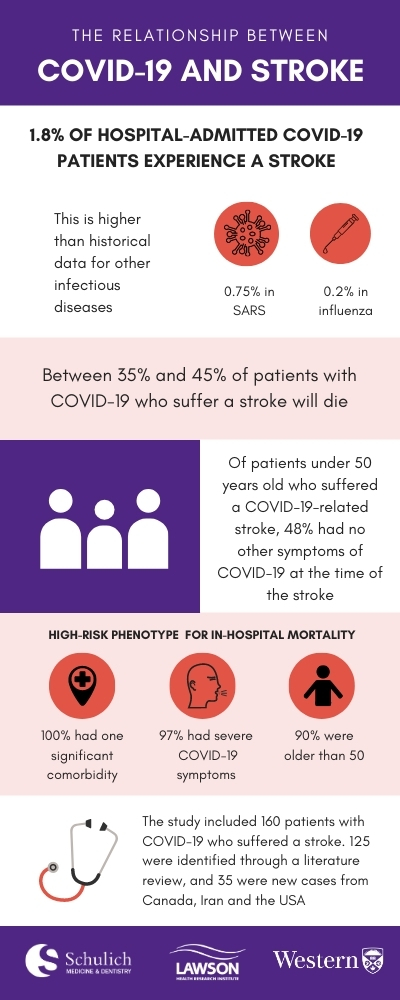
“One of the most eye-opening findings of this study is that for patients under 50 years old, many were totally asymptomatic when they had a stroke related to COVID-19. This means that for these patients, the stroke was their first symptom of the disease,” said Dr. Sposato, Associate Professor and the Kathleen and Dr. Henry Barnett Chair in Stroke Research at Western’s Schulich School of Medicine & Dentistry, and Scientist at Lawson.
Sposato says understanding the interplay between COVID-19 and stroke is important for treatment planning, especially in areas where COVID-19 is actively circulating in the community.
“The take-home message here for health care providers is that if you are seeing a patient with a stroke, particularly in those under 50 years old with large clots, you need to think of COVID-19 as a potential cause even in the absence of respiratory symptoms,” said Dr. Sposato.
The research team completed a systemic review of published cases of COVID-19 and stroke and pooled that data with another 35 unpublished cases from Canada, the USA and Iran. In total, the team examined 160 cases, looking at both clinical characteristics and in-hospital mortality.
“COVID-19 has changed the stroke landscape worldwide. As stroke neurologists, we need a new mindset to be able to promptly diagnose and treat patients with COVID-19 related strokes,” said Dr. Sebastian Fridman, Assistant Professor, Clinical Neurological Sciences at Schulich Medicine & Dentistry, research fellow at Lawson and first author on the study.