

Psychiatric disorders are often difficult to diagnose. As research advances, we are learning there are multiple subtypes of illness that differ in symptoms and treatment needs, making classification even harder. Post-traumatic stress disorder (PTSD) is one example. Individuals with the more common type of PTSD experience active defensive responses like hyperarousal or outbursts of emotion while those with the dissociative subtype experience additional passive defensive responses like ‘shutting down’ or out-of-body experiences.
In a new study from Lawson Health Research Institute and Western University, researchers combined brain imaging and machine learning to classify with 92 per cent accuracy whether individuals had PTSD and whether or not it was the dissociative subtype. The results highlight the promise of brain imaging as a tool for early diagnosis of psychiatric illness, helping to predict symptom development and treatment needs.
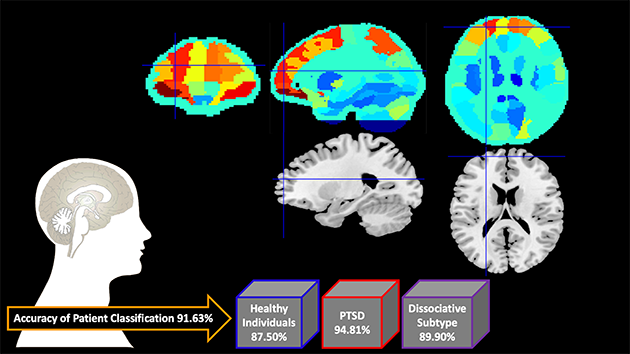
Brains scans and machine learning were combined to classify PTSD with 92 per cent accuracy.
The study involved 181 research participants, including those diagnosed with the more common form of PTSD, the dissociative subtype of PTSD, and healthy individuals with no history of PTSD. They participated in functional magnetic resonance imaging (fMRI) at St. Joseph’s Health Care London and Robarts Research Institute.
Researchers used the high-powered imaging to analyze patterns of resting-state brain activity where participants simply remained in a state of restful wakefulness in an fMRI scanner. The team found that unique patterns of brain activity differed significantly between the three groups.
“Our research group has been leading a number of studies that have shown differences in brain activity and neural connections between healthy individuals and those with different subtypes of PTSD,” says Dr. Ruth Lanius, a researcher at Lawson, professor at Schulich School of Medicine & Dentistry at Western University and psychiatrist at London Health Sciences Centre. “This study further validates that unique patterns of brain activity are associated with different forms of PTSD.”
In the second part of the study, the research team inputted the patterns of brain activity into a machine learning computer algorithm. They found the machine learning system could analyze brain scans to predict whether an individual had PTSD, the dissociative subtype of PTSD or no PTSD with 92 per cent accuracy.
“Our study suggests brain activity can be used to assist diagnosis of psychiatric disorders and help predict symptoms,” says Andrew Nicholson, PhD, lead author on the study and a post-doctoral fellow at Schulich Medicine & Dentistry who is conducting research at Lawson. “Patterns of brain activity are objective biomarkers that could be used to diagnose PTSD and, with more research, even predict response to treatment.”
Objective biomarkers hold promise for transforming psychiatric medicine.
“The field of psychiatry does not currently have objective biomarkers like those used to diagnose and understand other illnesses or diseases like cancer,” says Nicholson. “By discovering and validating patterns of brain activity as biomarkers, we can bring objective measures to psychiatry and transform patient care.”
The study, “Machine learning multivariate pattern analysis predicts classification of posttraumatic stress disorder and its dissociative subtype: A multimodal neuroimaging approach,” is published in Psychological Medicine.