

Representatives from the Council of Academic Hospitals of Ontario travelled to London, Ontario on January 20, 2017 for a special tour of Lawson Health Research Institute.
Lawson scientists showcased how hospital-based research plays a leading role in making Ontario healthier, wealthier, and smarter. Those on the tour or following the live social media posts were able to go behind-the-scenes and see how researchers are driving the future of health care for the community while growing our knowledge economy.
“As the research institute of London Health Sciences Centre and St. Joseph’s Health Care London, we are part of an important family. It’s research-based hospitals in Ontario that bridge the gap between discovery and the next generation of health service and delivery,” says Dr. David Hill, Scientific Director, Lawson.
Lawson believes that investment in health research is good for patients because research creates and improves treatments for better health outcomes and higher quality of life. It’s good for the economy as our researchers work on new services and improved procedures to drive efficiency and reduce costs. And, it is good for the community because London is gaining the reputation as a leader in the life sciences sector, attracting the best and brightest.”


The tour kicked-off with an event in the morning to celebrate the world-class health research enterprise in London. Leaders, staff, researchers, board members and other health research champions from Lawson, LHSC, St. Joseph’s and partners such as Western University gathered for the occasion.
We were honoured to welcome Councillor Harold Usher from the City of London. One of the priorities of London’s Community Economic Road Map is to develop a national centre of excellence for medical innovation and commercialization.
Also joining the kick-off and morning tour stops were Karen Vecchio, the federal Member of Parliament for Elgin-Middlesex-London and Official Opposition Critic for Families, Children and Social Development, and Jeff Yurek, Ontario’s Member of Provincial Parliament for Elgin-Middlesex-London and Health Critic.
Two research patients were there to share their experience. Wayne Kristoff has been participating in a clinical trial at St. Joseph’s Hospital aimed to induce the remission of type 2 diabetes. Since being involved with the study, Kristoff has been off all of his medication and has also experienced more energy and weight loss with the support offered by the research team.
Michael Allen is a two-time cancer survivor who recently celebrated 20 years of remission. He also underwent robotically-assisted heart surgery at LHSC’s University Hospital. During his recovery and rehabilitation, he was involved with personalized medicine research. Analysis of Allen’s individual makeup and drug response ensured he was receiving the right medication.
Centre for Clinical Investigations and Therapeutics (CCIT) with Dr. Richard Kim


Sue Tereschyn gave a tour of the lab space and an overview of the many types of studies that take place there, such as those researching treatments for diabetes, epilepsy and bariatrics.
CCIT is a state-of-the-art clinical research facility that enables pioneering discoveries through translational clinical research that improve patient care. As the first of its kind in Canada, this centre functions as a dedicated and centralized hub of the intellectual and physical resources needed by clinician researchers. It also has the capability for industry-sponsored clinical trials.
Dr. Wendy Teft explained a personalized medicine study focused on lessening the severity of side effects from taking chemotherapy for colorectal cancer.
Personalized Medicine with Dr. Richard Kim
Personalized Medicine is an emerging field that uses an individual’s genetic profile, medical history, environment and lifestyle to guide decisions related to the prevention, diagnosis and treatment of disease.


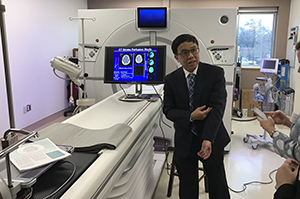
During the tour, equipment in the analytical lab (right) was being used to test safe drug treatment levels for a pregnant patient with a tumour.
At Lawson the focus has been on pharmacogenomics-based personalized medicine. This involves analyzing how the body is processing and using a drug, and then specifically adapting the treatment approach. The result is that people receive the right dose of the right drug, which better treats their condition and lessens the risk of an adverse drug reaction.
Drug levels are measured using mass spectrometry, a chemistry technique that identifies the amount and type of chemicals present in the blood, and analysis is done with the help of computer software.
The afternoon started with Dr. Frank Prato giving an overview of Lawson Imaging. This research group is a recognized leader in non-invasive biomedical imaging with new developments in hybrid imaging platforms such as MR/PET, PET/CT and SPECT/CT, currently being applied to the areas of cardiology, neurology, mental health, metabolic disease and cancer.
Dr. Savita Dhanvantari highlighted the opportunities for students and trainees in this highly collaborative research environment. Lawson Imaging has the expertise and creativity to innovate through basic research, translational research, clinical trials and commercialization.

Some members of the group donned lab coats to visit the Nordal Cyclotron & PET Radiochemistry Facility with Drs. Mike Kovacs, Savita Dhanvantari and Jonathan Thiessen (shown left). Positron-emitting radiopharmaceuticals (PERs) are produced to be used when patients undergo a PET scan. The facility produces short-lived PERs for St. Joseph’s Health Care London and is becoming the centre of a regional distribution network.
Meanwhile, the rest of the group learned about CT Perfusion with Dr. Ting-Yim Lee (shown right). CT Perfusion allows existing CT scanners in hospitals to measure tissue blood flow via a software program developed in Dr. Lee's lab. CT perfusion has benefits for stroke, cancer and heart attack, and is now used in over 4,000 hospitals worldwide.
The tour then headed across the city to meet with teams from Parkwood Institute Research. Cognitive Vitality and Brain Health, Mobility and Activity, and Mental Health form the three major research programs, with considerable overlap and synergies.
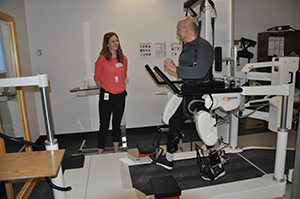

Nephrology research with Dr. Chris McIntyre
The Lilibeth Caberto Kidney Clinical Research Unit (KCRU) is a 4,000 square-foot facility dedicated to clinical research in the areas of kidney health, kidney disease and treatments of dialysis and kidney transplantation.

With a strong ongoing collaboration with the ICES Kidney Dialysis and Transplant Program, under the direction of Dr. Amit Garg, the two programs developed and delivered the MY TEMP trial of dialysis fluid cooling. At over 7000 patients this is the largest study of dialysis patients ever done.
Dialysis is a critical for patients, but is also expensive for the health care system and can cause many adverse effects due to the stress on the body’s organs. The team looks to improve dialysis and reduce its effects, and develop other interventions to treat kidney disease.
Cancer research with Dr. Gabe DiMattia
The Cancer Research Laboratory Program is a translational science enterprise moving clinically relevant laboratory discoveries to the clinic. Their goal is to broaden knowledge of cancer leading to the development of new treatment and detection strategies.


Dr. Samuel Asfaha is a Lawson clinical scientist and also practices gastroenterology as a physician. His research looks at inflammatory bowel disease and colorectal cancer. This includes looking at the origin cancer in the gut and which cells are involved, and the link between inflammation and cancer.
In his lab, scientists can isolate a single cell to grow a “mini gut” that is either normal or cancerous. They can even grow a cell from colon cancer and then study a cancerous tumour!
We had quick stop in the Gerald C. Baines Centre for Translational Cancer Research, an 11,000 square-foot centre that provides unique facilities to enable the work of cancer researchers and clinicians in London.
Dr. Aaron Ward and his research team focus on the development of sophisticated image techniques to further improve image-guided diagnostic procedures and therapy for cancer patients.
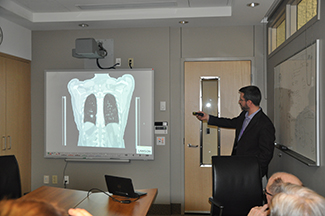
He discussed research that is working to better determine which patients need salvage therapy or surgery after radiation, which can be risky. They’ve developed an enhanced technology-driven analysis tool that can be used by clinicians in making this difficult decision.
Children’s Health Research Institute with Dr. Kathy Speechley
The Children’s Health Research Institute (CHRI) has a long and proud history of discovering ways to prevent and treat diseases affecting infants, children and youth, and to determine ways to promote happy, healthy lives.
Dr. Nathalie Berube spoke about the research program in neurodevelopment disorders, including intellectual disability, autism and schizophrenia. They work on better understanding of related genetics and the mechanisms of learning and memory, with the potential to identify new treatments to improve the quality of life for patients.


Dr. Barbra deVrijer is an obstetrics and gynecology physician whose research is inspired by her experience in the clinic with pregnant women. She noticed that over time the population has changed, with different lifestyles and higher rates of stress and obesity. New research and scanning methods are needed to monitor baby’s growth and development.
She teamed up with Dr. Charles McKenzie to develop a revolutionary way to obtain detailed images to look at the health of the placenta and fetus, measuring blood flow and distribution, fetal fat and signs of stress. It is the first lab in the world to image placental metabolism using MRI, which is radiation-free.